Articles
- Page Path
- HOME > Ann Occup Environ Med > Volume 38; 2026 > Article
- Review Impacts of heat on sleep quality among heat-exposed workers: a systematic review
-
Maarthi Raja1
 , Vidhya Venugopal1,*
, Vidhya Venugopal1,* , D. C. Mathangi2
, D. C. Mathangi2 , Suvarna Jyothi Kantipudi3
, Suvarna Jyothi Kantipudi3 , K. Mahesh Kumar4
, K. Mahesh Kumar4 , Somnath Panda1
, Somnath Panda1 , Latha Perumal Kamalakkannan1
, Latha Perumal Kamalakkannan1
-
Annals of Occupational and Environmental Medicine 2026;38:e3.
DOI: https://doi.org/10.35371/aoem.2026.38.e3
Published online: January 8, 2026
1Faculty of Public Health, Department of Environmental Health Engineering, Sri Ramachandra Institute of Higher Education and Research, Chennai, India
2Department of Mind Body Medicine & Lifestyle Sciences, Sri Ramachandra Faculty of Allied Health Sciences, Sri Ramachandra Institute of Higher Education and Research, Chennai, India
3Department of Psychiatry, Sri Ramachandra Institute of Higher Education and Research, Chennai, India
4Department of Physiology, Government Naturopathy and Yoga Medical College, The Tamil Nadu Dr. M.G.R. Medical University, Chennai, India
- *Corresponding author: Vidhya Venugopal NIHR GHRC NCD-EC, Faculty of Public Health, Department of Environmental Health Engineering, Sri Ramachandra Institute of Higher Education and Research (DU), No. 1, Ramachandra Nagar, Porur, Chennai, Tamil Nadu 600116, India E-mail: vvidhya@ehe.org.in
© 2026 Korean Society of Occupational & Environmental Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (https://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 2,219 Views
- 157 Download
Abstract
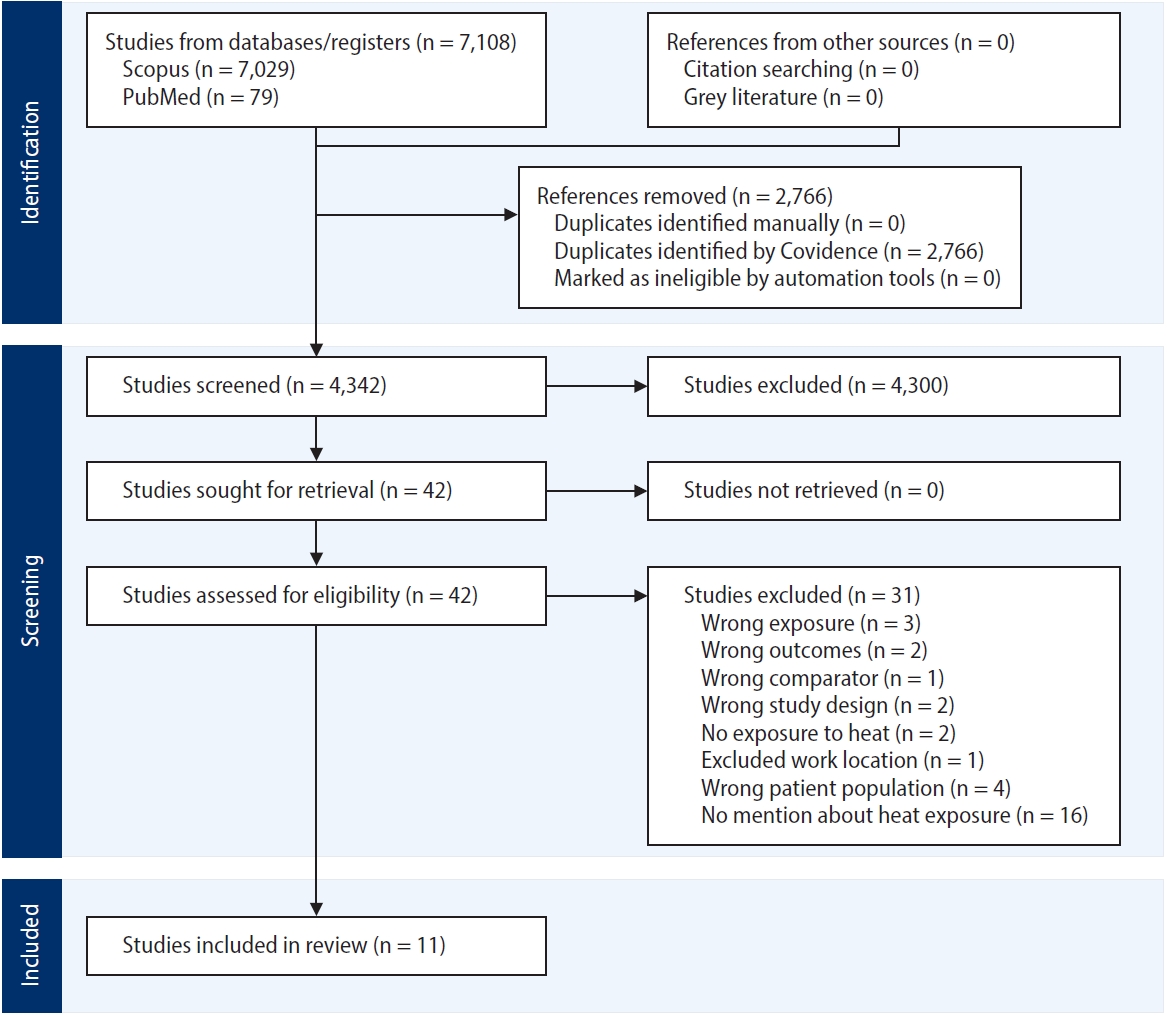
- Climate change is intensifying occupational heat exposure, posing risks not only for heat-related illness but also for sleep, which is essential for recovery, safety, and productivity. Heat-exposed workers are highly vulnerable due to prolonged exposure, limited access to cooling, and poor housing. This systematic review aimed to synthesise global evidence on how occupational heat exposure affects sleep quality among workers across different occupations and settings. A systematic review was conducted following Synthesis without Meta-Analysis (SWiM) guidelines. PubMed, Scopus, and Google Scholar were searched (2000–2025) for studies involving adult workers (≥18 years) reporting both heat exposure and sleep outcomes. The review was registered with PROSPERO (ID: CRD420251125735). Of 7,108 records screened, 11 studies met the inclusion criteria. Studies spanned Asia, Australia, North America, and global cohorts. Heat exposure consistently impaired sleep quality and duration. Using Pittsburgh Sleep Quality Index, Actigraphy, and self-reports, common complaints included difficulty falling asleep (64%), restlessness (54%), non-restorative sleep (54%), night sweats (36%), and reduced total sleep time (45%). Night-time temperatures above 25°C and high workplace wet bulb globe temperature values were strongly linked with reduced sleep efficiency and delayed sleep onset. Vulnerable groups included shift workers, petrochemical and steel labourers, women, older adults, and low-income workers in urban heat islands and poorly ventilated housing. Occupational heat exposure disrupts sleep, compounding daytime strain and creating a dual burden for workers. Integrating sleep into heat stress management through cooling interventions, better housing, and revised work–rest schedules is critical for workers well-being in a warming climate.
BACKGROUND
METHODS
RESULTS
DISCUSSION
CONCLUSIONS
Abbreviations
AC
CI
DL
JBI
KWCS
MD
ML
OR
PSQI
REM
RR
SE
TST
WASO
WBGT
-
Competing interests
No potential conflict of interest relevant to this article was reported.
-
Author contributions
Conceptualization: Raja M, Venugopal V. Data curation: Panda S, Kamalakkannan LP, Mathangi DC, Kantipudi SJ, Kumar KM. Formal analysis: Raja M. Investigation: Raja M, Panda S, Kamalakkannan LP. Methodology: Raja M, Venugopal V. Project administration: Raja M. Supervision: Raja M, Venugopal V. Validation: Venugopal V. Writing - original draft: Raja M, Panda S, Kamalakkannan LP. Writing - review & editing: Venugopal V.
-
Acknowledgments
The authors highly acknowledge and thank the Department of Environmental Health Engineering, Sri Ramachandra Institute of Higher Education and Research, Chennai, for providing us with this platform for carrying out the work. The authors also acknowledge the NIHR-Global Health Research Centre award scheme (Grant number GHRC for NCDs and EC: NIHR203247), using UK international development funding from the UK Government to support global health research. The views expressed in this publication are those of the authors and not necessarily those of the NIHR or the UK government.
NOTES
SUPPLEMENTARY MATERIAL
Supplementary Table 1.
Supplementary Table 2.
Supplementary Table 3.
| Study | Country | Study design | Sample size | Population (occupation/setting) | Exposure measure (WBGT, temperature) | Sleep measure (PSQI, actigraphy, diary) | Key finding | Effect estimate (OR/RR/β/MD) |
|---|---|---|---|---|---|---|---|---|
| Wu et al. (2024)23 | China | Cross-sectional | 952 | Petrochemical workers (enterprise) | WBGT | PSQI, total score; cutoff = 7 used to classify “sleep disorders” | 41.9% Prevalence; risk higher with >40 hour/week, heat, stress | No OR/RR/β/MD reported |
| Minor et al. (2022)27 | Global (68 countries) | Observational (wearable + climate data) | 7M+ sleep records | Workers and general population (68 countries) | Ambient temperature | Actigraphy (wearable fitness bands), total night-time sleep (minutes); sleep onset/offset; and short-sleep binary indicators using standard thresholds <7 hours, <6 hours, <5 hours | Night-time temp >25°C reduces sleep, increases insufficient sleep risk | MD: 1°C rise → ~5–10 minutes loss of sleep (varies by age/sex) |
| Hyun (2024)28 | Korea | National cross-sectional survey | 2,822 | General workforce (nationwide) | Not mentioned about exposure measurement | PSQI (Korean version); cut-off = 8.5 or more denotes presence of sleep disturbance | 49.9% Prevalence; risk higher with two-shift work, >53 hour/week, cold/heat symptoms | Paper reports associations between CHPI domains and sleep |
| Cheong and Gaynanova (2024)25 | USA | Observational (wearable sensing, mixed models) | 30 | Low-income, predominantly Black adults, Houston | Ambient temperature | Actigraphy (GENEActiv: sleep efficiency, TST) | 1°C Rise → ~2% decrease in sleep efficiency; AC mitigated effects | β = −2% sleep efficiency per 1°C increase (AC reduces effect) |
| Legault et al. (2017)26 | Canada | Field study, longitudinal (28–30 days) | 19 | Male underground miners, rotating shifts | Ambient conditions + WBGT (temp, humidity) | Actigraphy (TST, SE, WASO) + PSQI + sleep logs | Poor sleep vs. norms; 61% poor sleepers; degraded attention during night shifts under heat stress | No OR/RR/β/MD reported |
| Park et al. (2022)29 | Korea | Cross-sectional survey (KWCS) | 29,213 | Paid Korean workers (varied industries) | WBGT | Self-report (difficulty falling/maintaining sleep, fatigue) | Severe high-temperature exposure and sleep disturbance (OR: 3.09 in men; 3.30 in women); dose-response effect | OR (severe high temperature): men = 3.09 (95% CI: 2.69–3.56); women = 3.30 (95% CI: 2.81–3.87) |
| Magee et al. (2019)20 | Australia | Cross-sectional survey + Latent Class Analysis (LCA) | 542 employees (aged 18–60) | Australian employees, various sectors | Didn’t mention heat exposure measurement | Bed/wake times, sleep duration (work vs. non-work days), perceived sleep quality | Regular exposure to environmental stressors was linked to insufficient sleep (OR: 3.15) and “owls” (late sleepers; OR: 3.47) | ORs: Regular exposure class associated with insufficient sleep (OR: 3.15; 95% CI: 1.29–7.66) and with owls (OR: 3.47; 95% CI: 1.24–9.71) |
| Rasyid (2023)21 | Indonesia | Cross-sectional | 31 | Rolling mill steel industry workers | Work climate (WBGT) | PSQI, total score; cut off <5 = good sleep; ≥5 = poor sleep (they state PSQI <5 good, >5 poor) | Physical workload (p = 0.031), poor sleep quality (p = 0.047), hot climate (p = 0.002), and high noise (p = 0.009) were significantly associated with work fatigue | No OR/RR/β reported; associations only by p-values: physical workload vs. fatigue (p = 0.031) and sleep quality vs. fatigue (p = 0.047) |
| Minor et al. (2020)12 | 68 Countries worldwide | Observational, panel data analysis | 47,628 Adults, ~7 million nightly sleep records | Workers and general population (accelerometer users) | Night-time outdoor temperature (weather station data) | Wrist-worn accelerometers (sleep duration, onset, offset). Insufficient sleep <7 hours. Heat-associated deviations analyzed in minutes | Hotter nights shortened sleep, especially in older adults and women | Effect estimates (β/MD/percentage-point): Very warm nights (>30°C) reduced sleep by ~14.1 minutes (CI: −17.6 to −10.6). Nights >25°C increased the probability of sleeping <7 hours by ~3.5 percentage points compared with baseline 5–10°C nights |
| Park et al. (2017)30 | South Korea | Case-series using compensation records | 47 Compensated cases (2010–2014) | Heat-exposed workers (construction, cleaning, agroforestry) | WBGT (estimated from meteorological data), heat wave, tropical night | Lack of sleep provided by tropical nights | 95.7% Cases occurred when WBGT exceeded threshold; 61.7% during heat waves | No OR/RR; 95.7% of heat-related cases occurred above WBGT threshold; 61% during heat waves |
| Zhang et al. (2024)24 | China | Cross-sectional survey with ML/DL modelling | 2,393 Valid participants | Petrochemical workers, Fujian Province | Self-reported “temperature discomfort” using a 6-item scale assessing how high temperatures affected work efficiency | Sleep quality and sleep onset difficulty (questionnaire) | 18.0% reported poor sleep; poor sleep linked with higher productivity loss | High temperature exposure (OR: 1.77; 95% CI: 1.12–2.81), weekly >40 hours (OR: 1.74; 95% CI: 1.09–2.82), occupational stress (OR: 2.67; 95% CI: 1.89–3.80) |
WBGT: wet bulb globe temperature; PSQI: Pittsburgh Sleep Quality Index; OR: odds ratio; RR: risk ratio; MD: mean difference; CHPI: Composite Heat Exposure Index; TST: total sleep time; AC: air conditioner; SE: sleep efficiency; WASO: wake after sleep onset; KWCS: Korean Working Conditions Survey; CI: confidence interval; ML: machine learning; DL: deep learning.
| Study | Setting | Environmental measure | Duration/Intensity | Sleep outcomes (PSQI, TST, SE) | Main findings |
|---|---|---|---|---|---|
| Cheong and Gaynanova (2024)25 | Urban, Houston, low-income housing | Person-specific ambient temperature; AC use; outdoor temperature (25–38°C) | 14 Days of continuous monitoring | Sleep efficiency ↓ 2% per °C rise | Vulnerable urban residents (low AC use, poor housing) had worse sleep |
| Park et al. (2022)29 | National (urban and rural) | Self-report workplace temperature (high/low) | Chronic workplace exposures | Sleep disturbance (self-report) | High-temp workplaces (often industrial/urban) had a stronger association with poor sleep |
| Wu et al. (2024)23 | Petrochemical enterprise (Hainan, China) | WBGT, workplace monitoring | Chronic high temp (≥25°C WBGT) | PSQI | Rural-born vs. urban-born workers |
| Park et al. (2017)30 | Korean heat-exposed workers (construction, cleaning, agroforestry) | WBGT, tropical night (>25°C), heat wave (≥33°C for 2+ days) | Acute heat illness episodes (2010–2014) | Lack of sleep inferred from tropical nights | 78.7% of heat-illness cases followed tropical nights, suggesting urban night heat worsens sleep and heat risk |
| Symptom/Complaint | No. of studies reporting | % of total (n = 11) |
|---|---|---|
| Difficulty falling asleep | 7 | 64 |
| Night sweats | 4 | 36 |
| Restlessness | 6 | 54 |
| Non-restorative sleep | 6 | 54 |
| Reduced total sleep time | 5 | 45 |
- 1. Intergovernmental Panel on Climate Change. Global Warming of 1.5°C: An IPCC Special Report on the Impacts of Global Warming of 1.5°C above Pre-industrial Levels and Related Global Greenhouse Gas Emission Pathways, in the Context of Strengthening the Global Response to the Threat of Climate Change, Sustainable Development, and Efforts to Eradicate Poverty. Geneva, Switzerland: Intergovernmental Panel on Climate Change; 2018.
- 2. World Meteorological Organization. The Global Climate 2011-2020: A Decade of Accelerating Climate Change. Geneva, Switzerland: World Meteorological Organization; 2023.
- 3. World Health Organization. Climate change and workplace heat stress: technical report and guidance. https://www.who.int/publications/i/item/9789240099814. Updated 2025. Accessed September 3, 2025 ArticlePubMedPDF
- 4. Kjellstrom T, Briggs D, Freyberg C, Lemke B, Otto M, Hyatt O. Heat, human performance, and occupational health: a key issue for the assessment of global climate change impacts. Annu Rev Public Health 2016;37:97–112.ArticlePubMed
- 5. Flouris AD, Dinas PC, Ioannou LG, Nybo L, Havenith G, Kenny GP, et al. Workers' health and productivity under occupational heat strain: a systematic review and meta-analysis. Lancet Planet Health 2018;2(12):e521–31.ArticlePubMed
- 6. Kjellstrom T, Freyberg C, Lemke B, Otto M, Briggs D. Estimating population heat exposure and impacts on working people in conjunction with climate change. Int J Biometeorol 2018;62(3):291–306.ArticlePubMedPDF
- 7. Parson K. Human Thermal Environments: The Effects of Hot, Moderate, and Cold Environments on Human Health, Comfort, and Performance. 3rd ed. Boca Raton, FL: CRC Press; 2014.
- 8. Glaser J, Hansson E, Weiss I, Wesseling C, Jakobsson K, Ekstrom U, et al. Preventing kidney injury among sugarcane workers: promising evidence from enhanced workplace interventions. Occup Environ Med 2020;77(8):527–34.ArticlePubMedPMC
- 9. Johnson RJ, Sanchez-Lozada LG, Newman LS, Lanaspa MA, Diaz HF, Lemery J, et al. Climate change and the kidney. Ann Nutr Metab 2019;74 Suppl 3:38–44.ArticlePubMedPDF
- 10. Medic G, Wille M, Hemels ME. Short- and long-term health consequences of sleep disruption. Nat Sci Sleep 2017;9:151–61.ArticlePubMedPMCPDF
- 11. Krauchi K, Deboer T. The interrelationship between sleep regulation and thermoregulation. Front Biosci (Landmark Ed) 2010;15(2):604–25.ArticlePubMed
- 12. Minor K, Bjerre-Nielsen A, Jonasdottir SS, Lehmann S, Obradovich N. Ambient heat and human sleep. http://arxiv.org/abs/2011.07161. Updated 2020. Accessed September 3, 2025.
- 13. Ding R, Wang Y, Yu Y, Meng X, Gong Q, Tang Y, et al. Effectiveness of a multifaceted intervention (TEMP) for prevention of occupational heat-related illness among outdoor workers in the power grid industry: a cluster randomized controlled trial. Environ Health Perspect 2025;133(1):17001.ArticlePubMedPMC
- 14. Grandner MA. Sleep, health, and society. Sleep Med Clin 2022;17(2):117–39.ArticlePubMed
- 15. Gong L, Wang L, Hu R, Lu X, Sun Y, Zhang S, et al. Identification of unique ecosystem service bundles in farmland: a case study in the Huang-Huai-Hai Plain of China. J Environ Manage 2024;370:122516.ArticlePubMed
- 16. Sahu S, Sett M, Kjellstrom T. Heat exposure, cardiovascular stress and work productivity in rice harvesters in India: implications for a climate change future. Ind Health 2013;51(4):424–31.ArticlePubMed
- 17. International Labour Organization. Increase in heat stress predicted to bring productivity loss equivalent to 80 million jobs. http://www.ilo.org/global/about-the-ilo/newsroom/news/WCMS_711917/lang--en/index.htm. Updated 2019. Accessed September 15, 2023.
- 18. Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev 2021;10:89.PubMedPMC
- 19. Hilton M. JBI Critical appraisal checklist for systematic reviews and research syntheses. J Can Health Libr Assoc 2024;45(3):180–3.PMC
- 20. Magee C, Gopaldasani V, Bakand S, Coman R. The physical work environment and sleep: a latent class analysis. J Occup Environ Med 2019;61(12):1011–8.PubMed
- 21. Rasyid MF. Relationship between physical workload, sleep quality, work climate, and noise level with work fatigue in rolling mill workers in Sidoarjo steel industry. Indones J Public Health 2023;17(2):319–30.ArticlePDF
- 22. Park JS, Park EK, Kim HK, Choi GS. Prevalence and risk factors of occupational skin disease in Korean workers from the 2014 Korean Working Conditions Survey. Yonsei Med J 2020;61(1):64–72.ArticlePubMedPMCPDF
- 23. Wu Q, Fan S, Zhou B, Lu C, Zhang N, Su Z, et al. Relationship between occupational factors and sleep disorders among petrochemical workers on Hainan Island, South China: a cross-sectional study. Int J Occup Med Environ Health 2024;37(6):591–601.ArticlePubMedPMCPDF
- 24. Zhang Y, Chen Y, Su Q, Huang X, Li Q, Yang Y, et al. The use of machine and deep learning to model the relationship between discomfort temperature and labor productivity loss among petrochemical workers. BMC Public Health 2024;24(1):3269.ArticlePubMedPMCPDF
- 25. Cheong SM, Gaynanova I. Sensing the impact of extreme heat on physical activity and sleep. Digit Health 2024;10:20552076241241509.ArticlePubMedPMCPDF
- 26. Legault G, Clement A, Kenny GP, Hardcastle S, Keller N. Cognitive consequences of sleep deprivation, shiftwork, and heat exposure for underground miners. Appl Ergon 2017;58:144–50.ArticlePubMed
- 27. Minor K, Bjerre-Nielsen A, Jonasdottir SS, Lehmann S, Obradovich N. Rising temperatures erode human sleep globally. One Earth 2022;5(5):534–49.Article
- 28. Hyun MK. General worker's sleep disturbances and the degree of cold-heat symptoms: a national cross-sectional survey. J Pharmacopuncture 2024;27(3):199–210.ArticlePubMedPMC
- 29. Park I, Kim S, Kim Y, Yun B, Yoon JH. Association between physical risk factors and sleep disturbance among workers in Korea: the 5th Korean Working Conditions Survey. Sleep Med 2022;100:157–64.ArticlePubMed
- 30. Park J, Kim Y, Oh I. Factors affecting heat-related diseases in outdoor workers exposed to extreme heat. Ann Occup Environ Med 2017;29:30.ArticlePubMedPMCPDF
- 31. Okamoto-Mizuno K, Mizuno K. Effects of thermal environment on sleep and circadian rhythm. J Physiol Anthropol 2012;31(1):14.ArticlePubMedPMCPDF
- 32. Obradovich N, Migliorini R, Mednick SC, Fowler JH. Nighttime temperature and human sleep loss in a changing climate. Sci Adv 2017;3(5):e1601555.ArticlePubMedPMC
- 33. Xiang J, Bi P, Pisaniello D, Hansen A. The impact of heatwaves on workers' health and safety in Adelaide, South Australia. Environ Res 2014;133:90–5.ArticlePubMed
- 34. Bragazzi NL, Garbarino S, Puce L, Trompetto C, Marinelli L, Curra A, et al. Planetary sleep medicine: studying sleep at the individual, population, and planetary level. Front Public Health 2022;10:1005100.ArticlePubMedPMC
- 35. Nabeel I, Caraballo-Arias Y, Perkison WB, McCarthy RB, Saberi P, Berenji M, et al. Proposed mitigation and adaptation strategies related to climate change: guidance for OEM professionals. J Occup Environ Med 2021;63(9):e650–6.ArticlePubMed
- 36. Lo JC, Ong JL, Leong RL, Gooley JJ, Chee MW. Cognitive performance, sleepiness, and mood in partially sleep deprived adolescents: the need for sleep study. Sleep 2016;39(3):687–98.ArticlePubMedPMC
- 37. Ashe N, Wozniak S, Conner M, Ahmed R, Keenan O, Demetres MR, et al. Association of extreme heat events with sleep and cardiovascular health: a scoping review. Syst Rev 2025;14(1):19.ArticlePubMedPMCPDF
- 38. National Institute for Occupational Safety and Health. NIOSH criteria for a recommended standard: occupational exposure to heat and hot environments. NIOSH criteria for a recommended standard: occupational exposure to heat and hot environments. https://books.google.com/books?hl=en&lr=&id=KxD6HGC86S8C&oi=fnd&pg=PR3&dq=Criteria+for+a+Recommended+Standard:+Occupational+Exposure+to+Heat+and+Hot+Environments&ots=-5ZG8jrbHw&sig=o9D5_6eUZzuBpksn5Tl8_RDUUPg. Updated 2018. Accessed September 8, 2025.
- 39. Threshold Limit Value for Chemical Substances and Physical Agents and Biological Exposure Indices. Cincinnati, OH: American Conference of Governmental Industrial Hygienists; 2024.
- 40. Sharma A. The Factory Act, 1948 and social security: concept of factory, manufacturing process, worker and occupier. Indian J Law Leg Res 2023;5(2):1.
REFERENCES
Figure & Data
REFERENCES
Citations

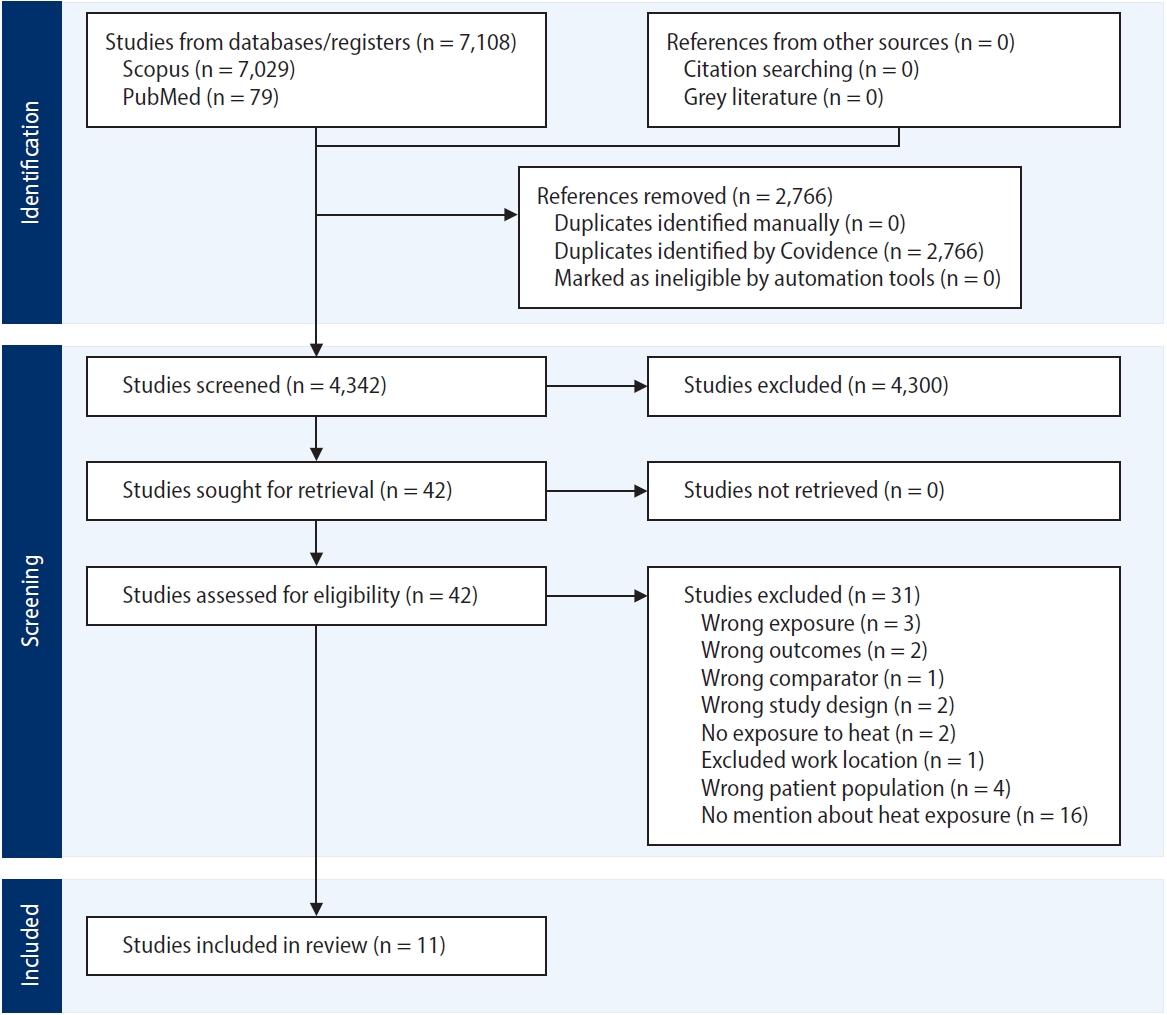
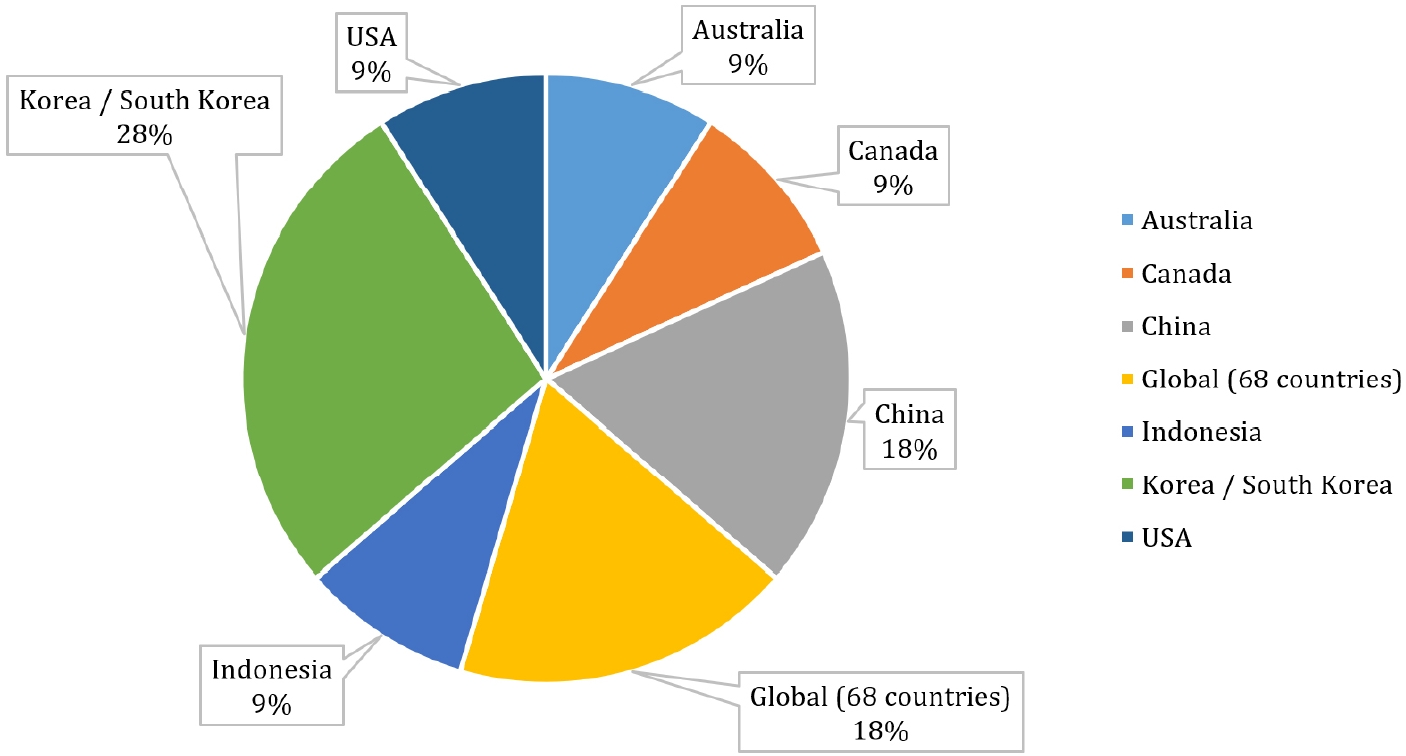
Fig. 1.
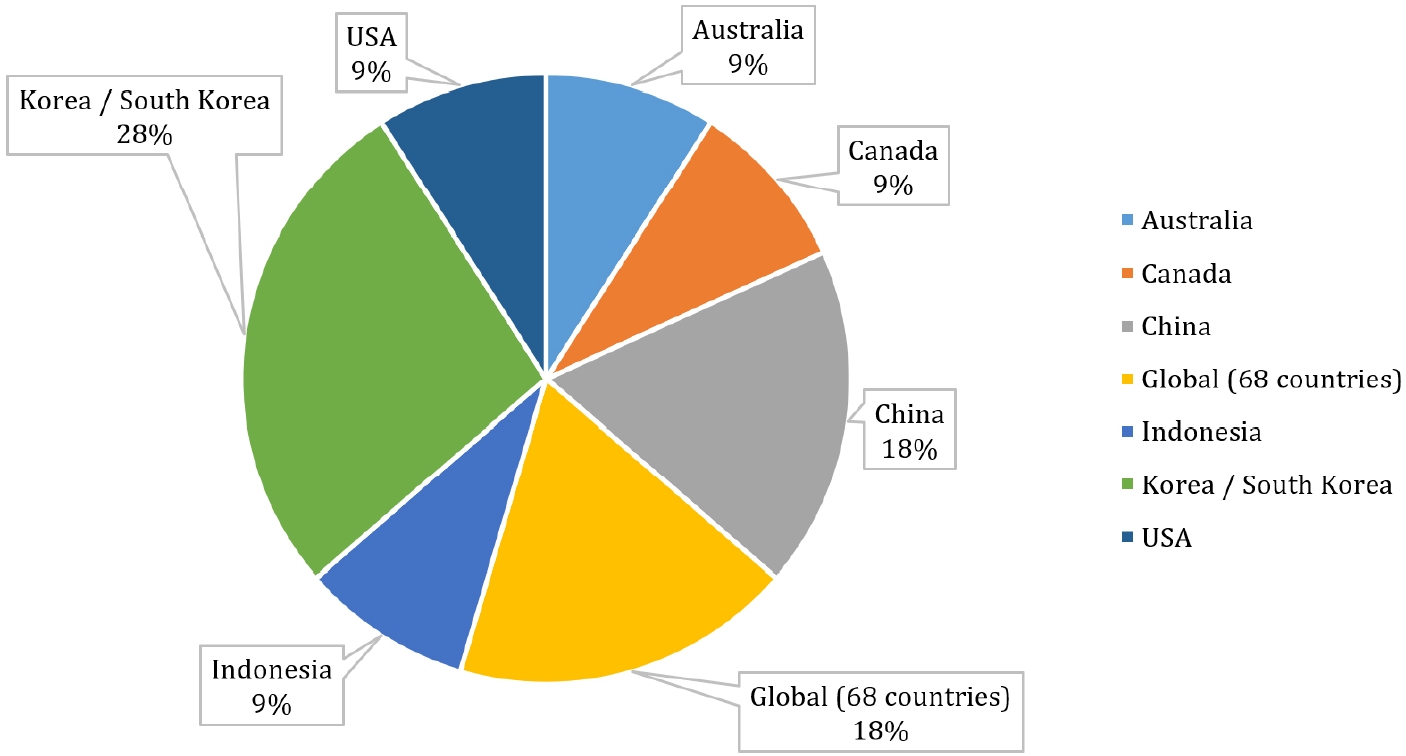
Fig. 2.
| Study | Country | Study design | Sample size | Population (occupation/setting) | Exposure measure (WBGT, temperature) | Sleep measure (PSQI, actigraphy, diary) | Key finding | Effect estimate (OR/RR/β/MD) |
|---|---|---|---|---|---|---|---|---|
| Wu et al. (2024)23 | China | Cross-sectional | 952 | Petrochemical workers (enterprise) | WBGT | PSQI, total score; cutoff = 7 used to classify “sleep disorders” | 41.9% Prevalence; risk higher with >40 hour/week, heat, stress | No OR/RR/β/MD reported |
| Minor et al. (2022)27 | Global (68 countries) | Observational (wearable + climate data) | 7M+ sleep records | Workers and general population (68 countries) | Ambient temperature | Actigraphy (wearable fitness bands), total night-time sleep (minutes); sleep onset/offset; and short-sleep binary indicators using standard thresholds <7 hours, <6 hours, <5 hours | Night-time temp >25°C reduces sleep, increases insufficient sleep risk | MD: 1°C rise → ~5–10 minutes loss of sleep (varies by age/sex) |
| Hyun (2024)28 | Korea | National cross-sectional survey | 2,822 | General workforce (nationwide) | Not mentioned about exposure measurement | PSQI (Korean version); cut-off = 8.5 or more denotes presence of sleep disturbance | 49.9% Prevalence; risk higher with two-shift work, >53 hour/week, cold/heat symptoms | Paper reports associations between CHPI domains and sleep |
| Cheong and Gaynanova (2024)25 | USA | Observational (wearable sensing, mixed models) | 30 | Low-income, predominantly Black adults, Houston | Ambient temperature | Actigraphy (GENEActiv: sleep efficiency, TST) | 1°C Rise → ~2% decrease in sleep efficiency; AC mitigated effects | β = −2% sleep efficiency per 1°C increase (AC reduces effect) |
| Legault et al. (2017)26 | Canada | Field study, longitudinal (28–30 days) | 19 | Male underground miners, rotating shifts | Ambient conditions + WBGT (temp, humidity) | Actigraphy (TST, SE, WASO) + PSQI + sleep logs | Poor sleep vs. norms; 61% poor sleepers; degraded attention during night shifts under heat stress | No OR/RR/β/MD reported |
| Park et al. (2022)29 | Korea | Cross-sectional survey (KWCS) | 29,213 | Paid Korean workers (varied industries) | WBGT | Self-report (difficulty falling/maintaining sleep, fatigue) | Severe high-temperature exposure and sleep disturbance (OR: 3.09 in men; 3.30 in women); dose-response effect | OR (severe high temperature): men = 3.09 (95% CI: 2.69–3.56); women = 3.30 (95% CI: 2.81–3.87) |
| Magee et al. (2019)20 | Australia | Cross-sectional survey + Latent Class Analysis (LCA) | 542 employees (aged 18–60) | Australian employees, various sectors | Didn’t mention heat exposure measurement | Bed/wake times, sleep duration (work vs. non-work days), perceived sleep quality | Regular exposure to environmental stressors was linked to insufficient sleep (OR: 3.15) and “owls” (late sleepers; OR: 3.47) | ORs: Regular exposure class associated with insufficient sleep (OR: 3.15; 95% CI: 1.29–7.66) and with owls (OR: 3.47; 95% CI: 1.24–9.71) |
| Rasyid (2023)21 | Indonesia | Cross-sectional | 31 | Rolling mill steel industry workers | Work climate (WBGT) | PSQI, total score; cut off <5 = good sleep; ≥5 = poor sleep (they state PSQI <5 good, >5 poor) | Physical workload (p = 0.031), poor sleep quality (p = 0.047), hot climate (p = 0.002), and high noise (p = 0.009) were significantly associated with work fatigue | No OR/RR/β reported; associations only by p-values: physical workload vs. fatigue (p = 0.031) and sleep quality vs. fatigue (p = 0.047) |
| Minor et al. (2020)12 | 68 Countries worldwide | Observational, panel data analysis | 47,628 Adults, ~7 million nightly sleep records | Workers and general population (accelerometer users) | Night-time outdoor temperature (weather station data) | Wrist-worn accelerometers (sleep duration, onset, offset). Insufficient sleep <7 hours. Heat-associated deviations analyzed in minutes | Hotter nights shortened sleep, especially in older adults and women | Effect estimates (β/MD/percentage-point): Very warm nights (>30°C) reduced sleep by ~14.1 minutes (CI: −17.6 to −10.6). Nights >25°C increased the probability of sleeping <7 hours by ~3.5 percentage points compared with baseline 5–10°C nights |
| Park et al. (2017)30 | South Korea | Case-series using compensation records | 47 Compensated cases (2010–2014) | Heat-exposed workers (construction, cleaning, agroforestry) | WBGT (estimated from meteorological data), heat wave, tropical night | Lack of sleep provided by tropical nights | 95.7% Cases occurred when WBGT exceeded threshold; 61.7% during heat waves | No OR/RR; 95.7% of heat-related cases occurred above WBGT threshold; 61% during heat waves |
| Zhang et al. (2024)24 | China | Cross-sectional survey with ML/DL modelling | 2,393 Valid participants | Petrochemical workers, Fujian Province | Self-reported “temperature discomfort” using a 6-item scale assessing how high temperatures affected work efficiency | Sleep quality and sleep onset difficulty (questionnaire) | 18.0% reported poor sleep; poor sleep linked with higher productivity loss | High temperature exposure (OR: 1.77; 95% CI: 1.12–2.81), weekly >40 hours (OR: 1.74; 95% CI: 1.09–2.82), occupational stress (OR: 2.67; 95% CI: 1.89–3.80) |
| Occupation group | Environmental exposure | Sleep outcomes | Common complaints | Key finding |
|---|---|---|---|---|
| Steel workers | WBGT 28–32°C, radiant heat | Poor PSQI scores | Night sweats, fatigue | Noise + heat interaction worsened outcomes |
| Petrochemical workers | Chronic WBGT exposure (indoor and outdoor tasks) | Higher PSQI (poorer quality) | Restlessness, insomnia, fatigue | Fatigue mediated by long heat exposure |
| Factory workers | Ambient temperature | Higher PSQI scores | Non-restorative sleep | Heat effects compounded by shift timing, similar to low-income workers in poorly ventilated housing |
| Labourers (manual/trades, including outdoor) | WBGT | Higher odds of insufficient sleep and “Owls” | Poor perceived sleep quality | OR: 6.40 (95% CI: 2.45–16.68); night heat reduced TST by ~7–15 minutes |
| General shift workers | WBGT | ~50% Prevalence of disturbed sleep | Poor recovery, insomnia | Survey evidence: vulnerable groups showed stronger effects (elderly, women, low-income) |
| Study | Setting | Environmental measure | Duration/Intensity | Sleep outcomes (PSQI, TST, SE) | Main findings |
|---|---|---|---|---|---|
| Cheong and Gaynanova (2024)25 | Urban, Houston, low-income housing | Person-specific ambient temperature; AC use; outdoor temperature (25–38°C) | 14 Days of continuous monitoring | Sleep efficiency ↓ 2% per °C rise | Vulnerable urban residents (low AC use, poor housing) had worse sleep |
| Park et al. (2022)29 | National (urban and rural) | Self-report workplace temperature (high/low) | Chronic workplace exposures | Sleep disturbance (self-report) | High-temp workplaces (often industrial/urban) had a stronger association with poor sleep |
| Wu et al. (2024)23 | Petrochemical enterprise (Hainan, China) | WBGT, workplace monitoring | Chronic high temp (≥25°C WBGT) | PSQI | Rural-born vs. urban-born workers |
| Park et al. (2017)30 | Korean heat-exposed workers (construction, cleaning, agroforestry) | WBGT, tropical night (>25°C), heat wave (≥33°C for 2+ days) | Acute heat illness episodes (2010–2014) | Lack of sleep inferred from tropical nights | 78.7% of heat-illness cases followed tropical nights, suggesting urban night heat worsens sleep and heat risk |
| Symptom/Complaint | No. of studies reporting | % of total (n = 11) |
|---|---|---|
| Difficulty falling asleep | 7 | 64 |
| Night sweats | 4 | 36 |
| Restlessness | 6 | 54 |
| Non-restorative sleep | 6 | 54 |
| Reduced total sleep time | 5 | 45 |
WBGT: wet bulb globe temperature; PSQI: Pittsburgh Sleep Quality Index; OR: odds ratio; RR: risk ratio; MD: mean difference; CHPI: Composite Heat Exposure Index; TST: total sleep time; AC: air conditioner; SE: sleep efficiency; WASO: wake after sleep onset; KWCS: Korean Working Conditions Survey; CI: confidence interval; ML: machine learning; DL: deep learning.
WBGT: wet bulb globe temperature; PSQI: Pittsburgh Sleep Quality Index; OR: odds ratio; CI: confidence interval; TST: total sleep time.
PSQI: Pittsburgh Sleep Quality Index; TST: total sleep time; SE: sleep efficiency; AC: air conditioner; WBGT: wet bulb globe temperature.
 KSOEM
KSOEM

 Cite
Cite

